Living with ulcerative colitis is a daily challenge for many people worldwide. Flare-ups, fatigue, and unpredictable symptoms can control your life. Medications help, but side effects and incomplete relief often leave you searching for more. In recent years, a growing number of patients and researchers are turning their attention to mushrooms—not as a culinary treat, but as a protocol for gut repair and immune modulation. Can mushrooms really help soothe the gut and balance immune function in ulcerative colitis? This guide explores the science, practical approaches, and real-world experience behind the mushroom protocol, aiming to offer new hope for those seeking a more holistic path to gut health.
What Is Ulcerative Colitis?
Ulcerative colitis (UC) is a chronic inflammatory bowel disease that mainly affects the colon and rectum. It causes inflammation and ulcers (sores) in the lining of the large intestine. Typical symptoms include:
- Frequent diarrhea, often with blood or pus
- Abdominal pain and cramping
- Urgent need to use the toilet
- Fatigue and weight loss
The exact cause is still unclear, but experts believe it involves an overactive immune response. Genetics, environment, and gut bacteria also play roles.
People with UC often face cycles of flare-ups and remission. Standard treatments include anti-inflammatory drugs, immune suppressants, and sometimes surgery. However, these options are not perfect. Side effects, cost, and incomplete symptom relief are common problems.
One thing that makes UC particularly frustrating is its unpredictability. Flare-ups can happen suddenly, sometimes triggered by stress, diet, or infection. The emotional impact is high—many people feel anxious about leaving home or planning activities, worried they might urgently need a bathroom.
Over time, this can affect work, relationships, and overall quality of life.
Medications like aminosalicylates, corticosteroids, and biologics are common, but not everyone responds well. Some people experience side effects such as headaches, nausea, or increased infection risk. Surgery to remove part of the colon is sometimes needed for severe cases, but this is a major step.
These challenges drive many to look for complementary approaches that can help restore balance and support healing from the inside out.
Why Consider Mushrooms For Ulcerative Colitis?
Mushrooms have been used in traditional medicine for thousands of years. In the last two decades, modern science has started to confirm their potential for gut repair and immune modulation. Here’s why mushrooms are capturing attention:
- Immune balancing: Mushrooms contain beta-glucans and other compounds that can both stimulate and calm the immune system.
- Gut barrier support: Some mushrooms help strengthen the gut lining, reducing “leaky gut.”
- Anti-inflammatory effects: Several types have natural substances that reduce inflammation without harsh side effects.
- Microbiome benefits: Certain mushrooms act as prebiotics, feeding good gut bacteria.
But not all mushrooms are equal. The right protocol involves choosing species with the best evidence, proper dosing, and timing.
One reason mushrooms stand out is their unique combination of nutrients and bioactive substances. Unlike single-compound drugs, mushrooms offer a range of compounds—polysaccharides, triterpenes, antioxidants, and more—that work together. This multi-targeted approach is helpful for complex diseases like UC, where inflammation, barrier damage, and immune confusion happen together.
Many people are surprised to learn that some mushrooms can actually help “train” the immune system, not just suppress or boost it. This makes them different from immune-suppressing drugs, which often leave you vulnerable to infections.
The Science Behind Mushrooms And Gut Health
Immune Modulation: Not Just Immune Boosting
Many people talk about “boosting” the immune system, but with UC, the immune system is already overactive in the wrong way. The real need is for immune modulation—helping the immune system react in a more balanced way.
Beta-glucans are special fibers found in the cell walls of mushrooms like shiitake, reishi, and turkey tail. These compounds interact with immune cells called macrophages and dendritic cells in the gut. Instead of just activating them, beta-glucans help the body increase “good” immune responses (like fighting infections) and decrease harmful ones (like attacking your own gut).
Several studies have shown that mushroom extracts can reduce the levels of TNF-alpha and interleukin-6—two chemical messengers that drive inflammation in UC.
Beyond clinical studies, practical experience shows that some people notice fewer infections, less allergic reaction, and even better responses to vaccines when using immune-modulating mushrooms. This suggests a more “intelligent” immune support, not just blunt suppression.
Gut Barrier Repair
The gut lining is like a fence, keeping good things in and bad things out. In ulcerative colitis, this “fence” gets damaged, leading to increased permeability (often called leaky gut). This allows toxins and bacteria to enter the bloodstream, making inflammation worse.
Mushrooms like lion’s mane contain compounds that stimulate the growth of new cells in the gut lining. Polysaccharides in other mushrooms can increase the production of mucin, which helps protect and rebuild the mucosal barrier.
Some research suggests that these compounds also encourage the release of growth factors such as nerve growth factor (NGF), which supports the nerves that help coordinate gut movement and healing. This may be one reason why some people report not only fewer symptoms but also improved digestion and even less sensitivity to certain foods.
Anti-inflammatory Action
Most anti-inflammatory drugs for UC come with risks. Mushrooms offer a gentler alternative. Triterpenes in reishi and ergothioneine in oyster mushrooms reduce inflammation without suppressing the entire immune system.
Animal studies and early human trials suggest that regular use of certain mushroom extracts can reduce colon inflammation, improve stool consistency, and help maintain remission.
Another advantage is that mushrooms can calm inflammation throughout the body, not just in the gut. For example, ergothioneine is a rare antioxidant found in oyster mushrooms that also supports the liver and blood vessels. This “whole-body” effect may explain why some users notice less joint pain or skin irritation as well.
Effects On Gut Microbiome
A healthy colon needs a healthy mix of bacteria. Mushrooms contain prebiotic fibers that feed good bacteria like bifidobacteria and lactobacilli. They also suppress harmful microbes, which can trigger flares. Some studies show that turkey tail and maitake mushrooms change the gut microbiome in ways that support healing.
Mushroom-derived prebiotics can increase short-chain fatty acids (SCFAs), such as butyrate. These SCFAs are important for nourishing the cells of the colon and reducing inflammation. People often overlook this indirect effect, but it can be a key part of restoring long-term balance.
Key Mushrooms Used In Protocols For Ulcerative Colitis
Not all mushrooms offer the same benefits. Here are the main species backed by research and experience:
1. Reishi (ganoderma Lucidum)
Reishi is known as the “mushroom of immortality” in Asia. It contains triterpenes and beta-glucans with strong immune-modulating effects.
- Key benefits: Reduces colon inflammation, balances immune response, supports liver detox.
- Research: Clinical studies show reishi extracts can lower pro-inflammatory cytokines and improve symptoms in IBD models.
- Typical dose: 1–3 grams per day of extract.
Reishi is often described as calming, not just for the gut but also for the mind. Many users report better sleep and less anxiety, which can be important for anyone with a chronic illness.
2. Lion’s Mane (hericium Erinaceus)
Lion’s mane is famous for brain health, but it’s also a star for gut repair.
- Key benefits: Stimulates gut lining regeneration, improves mucosal barrier, supports nerves that control the gut.
- Research: Animal studies show lion’s mane reduces colon damage and speeds healing in colitis.
- Typical dose: 1–2 grams per day of extract.
Lion’s mane is unique because it supports the gut-brain axis. Some people notice improved mood, focus, and even less “brain fog” when they use this mushroom regularly.
3. Turkey Tail (trametes Versicolor)
Turkey tail is one of the most studied mushrooms for immune support.
- Key benefits: Balances immune activity, increases beneficial gut bacteria, reduces oxidative stress.
- Research: Human and animal studies show improvements in immune markers and gut bacteria diversity.
- Typical dose: 2–3 grams per day of extract.
Turkey tail is a favorite for those recovering from antibiotics or seeking to rebuild a healthy microbiome after a flare.
4. Shiitake (lentinula Edodes)
Best known as a food, shiitake is also a gut-friendly mushroom.
- Key benefits: Contains lentinan (a beta-glucan) that supports gut lining and immunity.
- Research: Studies show shiitake extracts reduce colon inflammation and support healthy bacteria.
- Typical dose: 3–5 grams per day (fresh or extract).
Shiitake is often easier to find in grocery stores, making it a practical option for adding to meals as well as using extracts.
5. Maitake (grifola Frondosa)
Maitake is prized for its unique polysaccharides.
- Key benefits: Supports gut barrier, reduces inflammation, feeds good bacteria.
- Research: Early studies suggest improved immune balance and gut health in colitis models.
- Typical dose: 1–3 grams per day of extract.
Maitake also has mild blood sugar-lowering effects, which can be helpful for those with metabolic concerns related to chronic inflammation.
6. Chaga (inonotus Obliquus)
Chaga is rich in antioxidants.
- Key benefits: Protects cells from oxidative stress, may reduce damage to colon lining.
- Research: Animal studies show reduction in colon ulcers and inflammation.
- Typical dose: 1–2 grams per day of extract.
Chaga is often used in tea form, and some people find it soothing during stressful periods.
7. Oyster Mushroom (pleurotus Ostreatus)
Oyster mushroom is a good source of ergothioneine, a rare antioxidant.
- Key benefits: Calms inflammation, supports immune balance, improves gut flora.
- Research: Extracts show anti-inflammatory effects in gut models.
- Typical dose: 2–4 grams per day (fresh or extract).
Oyster mushrooms are also high in B vitamins and can add valuable nutrition to your diet.
How A Mushroom Protocol Works For Ulcerative Colitis
A mushroom protocol is not just eating mushrooms randomly. It’s a structured approach using extracts and powders in specific combinations, doses, and timing.
Building A Basic Protocol
A typical protocol might look like:
- Morning: Lion’s mane + turkey tail (gut repair + immune modulation)
- Midday: Shiitake or maitake (prebiotic support)
- Evening: Reishi (calming, anti-inflammatory, sleep support)
Duration: Most protocols last at least 8–12 weeks for best results.
Form: Extracts are usually more effective than whole mushrooms because they are concentrated and easier to absorb.
Protocols can be adjusted based on symptoms. For example, if you have more anxiety or trouble sleeping, you might increase reishi in the evening. If you’re struggling with diarrhea or frequent flares, focusing on lion’s mane and turkey tail can be helpful.
If you’re recovering from antibiotics, adding more prebiotic mushrooms like shiitake and maitake can speed microbiome recovery.
Sample Dosage Table
Here’s an example of how a daily protocol might be planned:
| Mushroom | Morning | Midday | Evening | Total per Day |
|---|---|---|---|---|
| Lion’s Mane | 1g | – | – | 1g |
| Turkey Tail | 1g | – | – | 1g |
| Shiitake | – | 2g | – | 2g |
| Reishi | – | – | 1g | 1g |
This plan is just a starting point. Some people add chaga or maitake, or rotate different mushrooms each week to avoid tolerance and cover more benefits.
Cycling And Adjustments
Some people cycle their mushrooms (e. g. , 5 days on, 2 days off) to prevent the body from adapting. Adjustments are made based on symptom changes, side effects, or lab tests.
Tip: Always start with lower doses and increase slowly to watch for reactions.
It’s also wise to introduce new mushrooms one at a time. This way, if you notice any discomfort, it’s easier to identify the cause. For example, you might add lion’s mane for two weeks, then turkey tail, then reishi.
Benefits Of The Mushroom Protocol For Gut Repair
Reduced Inflammation
Most users report less pain, cramping, and urgency after 4–6 weeks. This is backed by studies showing lower levels of C-reactive protein (CRP) and calprotectin (two markers of gut inflammation).
These benefits often build slowly. In many cases, flare-ups become shorter and less severe. For some, the urge to urgently find a restroom fades, and “good days” become more common.
Improved Gut Barrier
Mushrooms like lion’s mane and shiitake can help rebuild the gut lining. People notice:
- Fewer episodes of diarrhea
- Less blood in the stool
- Better tolerance to food
With a stronger gut barrier, you may also find you react less to trigger foods or stress. Over time, you might be able to enjoy a wider variety of foods without symptoms.
Enhanced Remission Periods
Some protocols help maintain remission for months or even years. The immune-modulating effects reduce the chances of sudden flares.
Longer remission means fewer trips to the doctor, less anxiety about surprise symptoms, and more stability in daily life. Many people find they can plan travel or social events with more confidence.
Better Energy And Mood
Chronic inflammation drains energy. By calming the gut, many users experience better sleep, more energy, and improved mental clarity.
Some mushrooms, especially reishi and lion’s mane, have mild calming effects. This can help with sleep issues and stress, which often trigger or worsen UC symptoms.
Less Medication Dependency
Although not a replacement for prescribed drugs, some patients find they need lower doses or fewer medications after several months on the protocol (always with doctor supervision).
This is especially valuable for people who struggle with medication side effects. Reducing dependency can also save money and simplify your routine.

Credit: www.frontiersin.org
Safety, Side Effects, And Who Should Avoid Mushroom Protocols
Safety Overview
Most medicinal mushrooms are safe for long-term use when taken in reasonable doses. Side effects are rare but can include:
- Mild digestive upset (bloating, gas)
- Allergic reactions (especially in people allergic to molds)
- Interactions with immunosuppressant drugs
Some people may notice changes in bowel movements or mild headaches during the first week. These usually fade as the body adjusts. Drinking enough water and starting with low doses can reduce these effects.
Who Should Avoid
- People with mushroom allergies: Any sign of rash, swelling, or breathing trouble means stop immediately.
- Transplant recipients or those on immune-suppressing drugs: Mushrooms may interact with these medications.
- Pregnant or breastfeeding women: There’s not enough research for these groups.
- People with autoimmune disorders outside the gut: Mushrooms can sometimes activate the immune system in ways that worsen other autoimmune diseases.
Tip: Always consult your healthcare provider before starting any new supplement, especially if you take medications.
It’s important to read ingredient labels carefully. Some mushroom blends contain added herbs or fillers. If you have food sensitivities, look for pure, single-species extracts.
Practical Insights: Getting The Most From A Mushroom Protocol
Choosing The Right Form
- Extracts: Most research uses concentrated extracts. Look for “hot water” or “dual extraction” for best results.
- Powders: Good for adding to smoothies or soups, but less potent than extracts.
- Capsules: Convenient and precise, but check for fillers or additives.
Extracts are usually best for therapeutic use. Hot water extracts pull out polysaccharides, while dual extracts also include alcohol to draw out triterpenes and other fat-soluble compounds. For best results, match the form to your goal. For example, if you want more immune support, dual extracts of reishi are ideal.
Quality Matters
Not all mushroom products are equal. Choose brands that:
- Test for heavy metals and pesticides
- Use fruiting bodies, not just mycelium (the root-like part)
- Provide third-party lab results
Ask for certificates of analysis or look for trusted third-party seals. Mushrooms can absorb toxins from the soil, so quality testing is essential.
Combining With Diet And Lifestyle
Mushrooms work best when combined with:
- Anti-inflammatory diet: Lots of vegetables, healthy fats, and low sugar
- Good sleep: Mushrooms like reishi can help calm the mind
- Stress management: Mindfulness, yoga, or gentle exercise
Hydration also matters. Drink plenty of water to support gut healing and help your body process mushroom extracts. Gentle movement, such as walking, can also help your gut motility.
What Beginners Often Miss
- Consistency is key: Mushrooms are not fast-acting like painkillers. Results build over weeks, not days.
- Start with one species: Adding too many at once can confuse your gut. Introduce new mushrooms slowly.
- Not all symptoms mean progress: Some people experience mild bloating or changes in stool at first. This can be a sign your gut bacteria are adjusting. It usually passes in 1–2 weeks.
Another common mistake is stopping at the first sign of discomfort. Minor digestive changes are normal as your gut adapts. If symptoms are mild, try lowering the dose before stopping completely.
Comparing Mushrooms To Conventional Treatments
To help you understand how mushrooms fit into the bigger picture, here’s a direct comparison:
| Aspect | Mushroom Protocol | Conventional Medication |
|---|---|---|
| Main action | Immune modulation, gut repair | Suppress inflammation, immune suppression |
| Side effects | Rare, mild (if any) | Common (nausea, infection risk, liver issues) |
| Long-term safety | Generally safe | May cause long-term complications |
| Onset of action | 4–8 weeks | Days to weeks |
| Remission maintenance | Promising, needs more research | Well established |
Note: Mushrooms are best used as a complement, not a replacement, for medical therapy.
One non-obvious insight: Even when medications work well, adding a mushroom protocol can help reduce side effects by supporting the liver and immune system.
Case Examples And Real-world Experience
Case 1: Mild Uc, Poor Response To Diet Alone
A 34-year-old woman with mild UC had frequent urgency and occasional blood. She started a protocol with lion’s mane and turkey tail, along with her usual anti-inflammatory diet.
- Results after 2 months: Less urgency, no visible blood, improved energy.
She also noticed better sleep and felt calmer during stressful workdays. These “side benefits” helped her stick with the protocol and maintain healthier habits.
Case 2: Moderate Uc, Flare After Antibiotics
A 42-year-old man experienced a flare after antibiotics wiped out his gut bacteria. He added reishi and shiitake extracts daily.
- Results after 6 weeks: Reduced cramping, firmer stools, fewer bathroom trips.
Interestingly, his doctor noted a drop in CRP levels, suggesting lower inflammation. He was able to return to work full-time without fear of sudden symptoms.
Case 3: In Remission, Looking To Prevent Flare
A 29-year-old woman in remission wanted to stay well. She used a rotating protocol (5 days on, 2 days off) with maitake, lion’s mane, and reishi.
- Results after 1 year: No flares, steady energy, and better sleep.
She also found her tolerance for occasional “treat” foods (like bread or cheese) improved, although she continued to eat mostly whole, plant-based meals.
Tip: Individual responses vary. Track your symptoms with a journal to see what works best for you.
Small changes, such as adding probiotics or adjusting the mushroom blend, can make a big difference in results.
How Mushrooms Support The Gut Microbiome
The balance of bacteria in your gut is crucial for colitis. Mushrooms:
- Feed beneficial bacteria (prebiotic effect)
- Reduce growth of “bad” bacteria linked to flares
- Increase short-chain fatty acid (SCFA) production, which helps heal the gut lining
In several studies, turkey tail and shiitake improved bifidobacteria numbers and reduced markers of inflammation in the colon.
You might notice changes in digestion—less bloating, better stool consistency, or even fewer food cravings. This is partly due to a healthier microbiome. Over time, a balanced microbiome can help “train” the immune system to be less reactive.
Common Mistakes When Using Mushrooms For Ulcerative Colitis
- Using culinary mushrooms only: While food mushrooms are healthy, medicinal extracts are much stronger.
- Choosing the wrong form: Some products use only mycelium, which is less potent than the fruiting body.
- Expecting overnight results: Gut repair takes time. Give at least 8–12 weeks before judging effectiveness.
- Ignoring interactions: Some mushrooms interact with blood thinners or immune drugs.
- Not tracking symptoms: Keep a daily log to notice patterns and adjust your protocol.
A less obvious mistake: Not rotating mushrooms or taking breaks. Long-term use of the same blend can sometimes lead to “diminishing returns.” Cycling mushrooms helps keep your body responsive.
The Role Of Mushrooms In Long-term Remission
Mushrooms are not a cure, but they may help some people:
- Extend remission periods
- Reduce severity of flares
- Improve resilience to stress and dietary slip-ups
Long-term use appears safe, but it’s wise to take occasional breaks and discuss your plan with a healthcare provider.
Another benefit is improved quality of life. People often feel less anxious about triggers, more confident in their daily routine, and better equipped to handle small setbacks.
How To Talk To Your Doctor About Mushroom Protocols
Many doctors are open to complementary therapies if you bring solid information. Share:
- Research studies on specific mushrooms
- Your reasons for trying the protocol
- A clear plan for monitoring symptoms and side effects
Ask your doctor to check for possible interactions with your current medications. Be honest about all supplements you’re taking.
Bringing a written list of questions and a symptom diary helps your doctor understand your experience and support your choices more effectively.

Credit: www.frontiersin.org
Realistic Expectations: What To Expect From A Mushroom Protocol
- First 2 weeks: Minor changes, possible digestive adjustment
- Weeks 3–6: Gradual reduction in pain, urgency, and stool frequency
- Weeks 7–12: Greater energy, improved gut tolerance, fewer flare signs
- Long-term: Potential for longer remission, less medication need, better resilience
Insight: Not everyone responds the same way. Genetics, diet, and lifestyle play a big role. Patience is key.
If you don’t see big changes in the first month, don’t give up. Subtle improvements, like more stable energy or better sleep, often come before major symptom relief.
Where To Find High-quality Mushroom Supplements
Look for companies that:
- Grow mushrooms organically, free from pesticides
- Use fruiting bodies, not just mycelium
- Provide third-party lab tests for potency and purity
- Offer clear dosing instructions
A helpful guide for evaluating supplements can be found at the ConsumerLab site.
Look for customer reviews, transparent sourcing, and responsive support. If you’re unsure, ask for recommendations from health professionals who understand mushroom protocols.
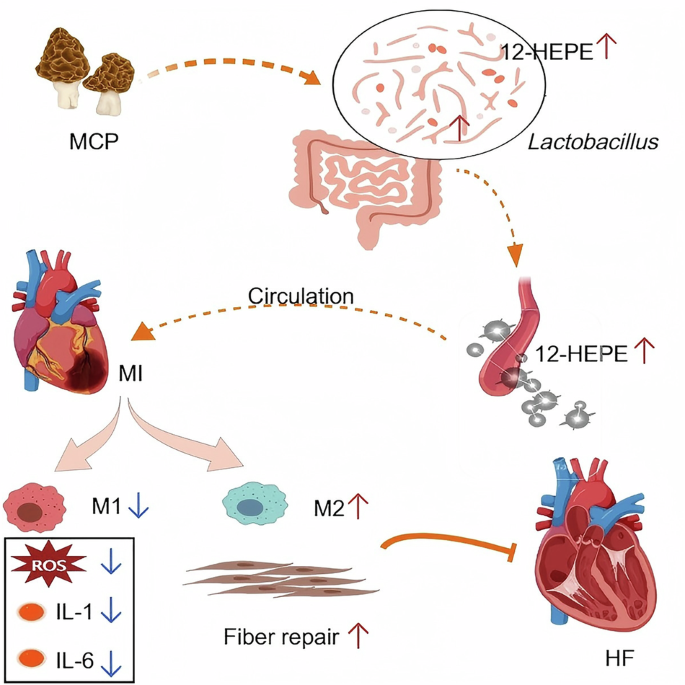
Credit: www.nature.com
Frequently Asked Questions
What Is The Best Mushroom For Ulcerative Colitis?
There’s no single “best” mushroom. Lion’s mane is excellent for gut lining repair, while reishi and turkey tail are strong for immune modulation. Many protocols use a combination for the best effect.
How Long Does It Take To See Results From The Mushroom Protocol?
Most people notice changes within 4–8 weeks, with bigger improvements after 12 weeks. Gut repair is slow and requires consistent use.
Are Mushroom Protocols Safe With Other Medications?
Generally, yes, but caution is needed with immune suppressants and blood thinners. Always check with your doctor before starting, as some interactions are possible.
Can I Eat Regular Mushrooms Instead Of Taking Extracts?
Culinary mushrooms are healthy, but extracts contain much higher levels of active compounds. For therapeutic results in UC, use standardized extracts or powders.
Should Children Or Elderly People Use Mushroom Protocols?
Most research is on adults. For children or the elderly, always consult a healthcare provider first. Doses may need to be adjusted for age and body weight.
Living with ulcerative colitis is never simple, but a structured mushroom protocol offers a new tool for those seeking gut repair and immune balance. With the right information, careful planning, and close monitoring, mushrooms may help many people feel stronger, more resilient, and in better control of their health journey. As research grows, so does the hope for a brighter, calmer future for anyone dealing with UC.